How Do Hospitals Set Prices for COVID-19 Lab Tests?

Hospitals Set Prices for COVID-19 Lab Tests
COVID-19 has dramatically impacted the hospital industry. As hospitals adjust to new challenges, they must also face questions about new procedures and treatment requirements. In our next two blog posts, we’ll take a close look at how hospitals are pricing COVID-19 lab tests and isolations rooms.
We sent out a survey to assess how hospitals were approaching this new pricing challenge and were pleased to receive 40 responses. In the midst of this challenging time, we appreciate this sharing of information!
We’ll first look at how hospitals are pricing COVID-19 lab tests. First, some context: On March 5 and February 13, CMS announced new HCPCS codes to test patients for SARS-CoV-2/2019-nCoV (COVID-19). Starting in April, laboratories using CDC tests are to use the U0001 code while non-CDC tests will use the U0002 code. Medicare payment has been established at $36 for U0001 and $51 for U0002. On April 15, reimbursement was increased to $100 for U0003 and U0004 for sites using high throughput technologies.
Our survey focused on how hospitals are developing CDM and cash pay pricing for these tests. Cash pay pricing is an important element as part of the stimulus package requires that providers post a cash pay price for these tests. Three key points emerged from the survey:
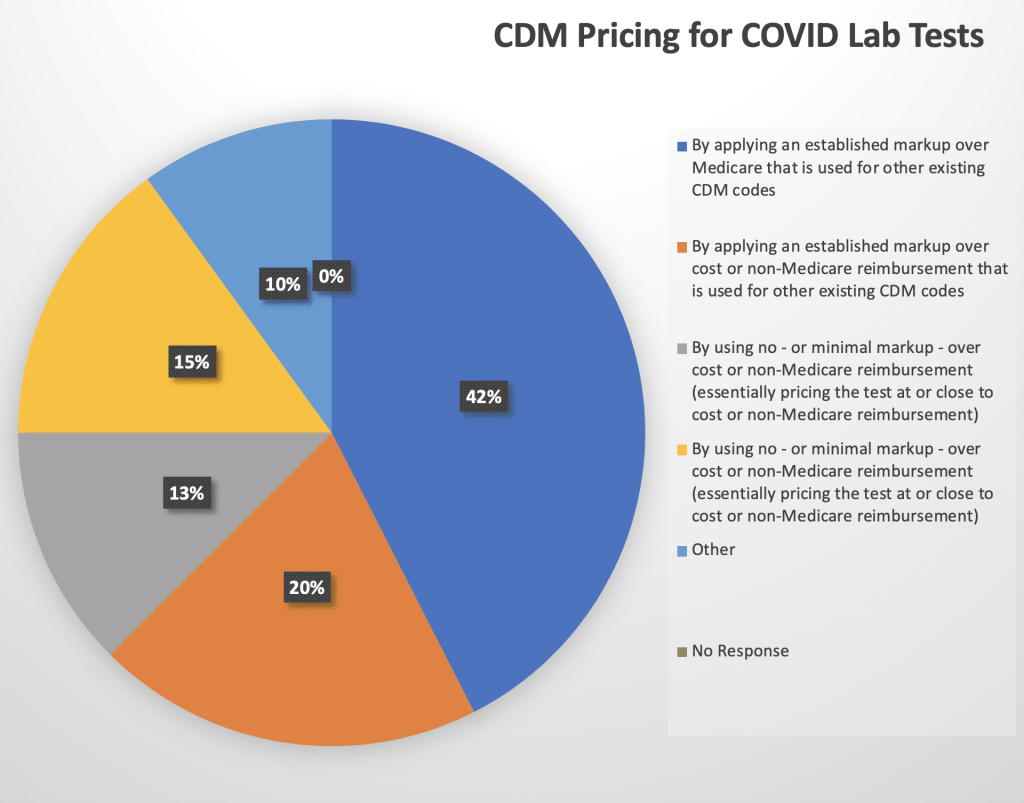
- CDM pricing:
- over 60% of respondents are using some markup over Medicare payment, cost, or non-Medicare reimbursement. Meaning, the majority are pricing these tests in a way that is likely consistent with other items in the CDM.
- 25% are essentially creating a CDM price that is virtually the same as the Medicare payment/cost/or non-reimbursement rate.
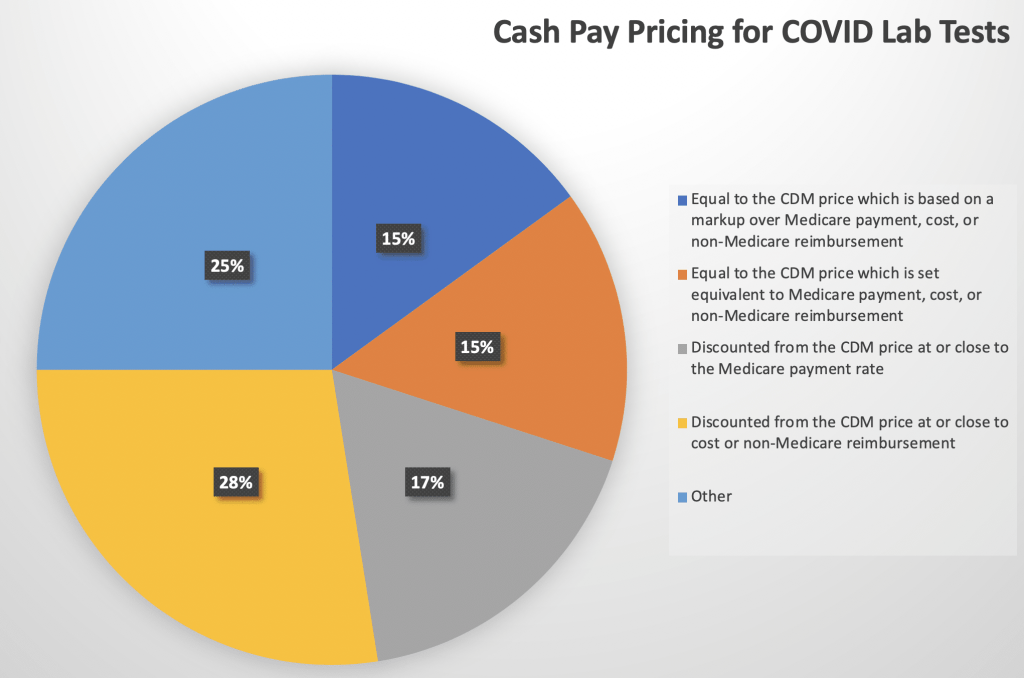
- Cash pay pricing: Roughly half are posting a cash pay price that is virtually the same as the Medicare payment/cost/or non-reimbursement rate.
- The combination of both points above make it clear that no one is trying to make money on these tests – just providing the ability to cover costs. Even those using a markup to create pricing appear to be setting rates such that when their payer discounts or self-pay policies are applied the end payment will be virtually the same as their cost.
If you’d like more information about our survey, or to take a look at the result, let us know!